Use Extraction Operator to Read in File
| Dental extraction | |
|---|---|
 Surgical extraction of an impacted molar | |
| ICD-nine-CM | 23.0-23.1 |
| MeSH | D014081 |
A dental extraction (too referred to as molar extraction, exodontia, exodontics, or informally, tooth pulling) is the removal of teeth from the dental alveolus (socket) in the alveolar os. Extractions are performed for a wide multifariousness of reasons, but most usually to remove teeth which have become unrestorable through molar decay, periodontal disease, or dental trauma, especially when they are associated with toothache. Sometimes impacted wisdom teeth (wisdom teeth that are stuck and unable to grow normally into the mouth) cause recurrent infections of the gum (pericoronitis), and may be removed when other conservative treatments have failed (cleaning, antibiotics and operculectomy). In orthodontics, if the teeth are crowded, good for you teeth may be extracted (frequently bicuspids) to create space and so the residue of the teeth can be straightened.
Procedure [edit]
Extractions could be categorized into not-surgical (simple) and surgical, depending on the type of molar to be removed and other factors.

A dental x-ray image (radiograph) showing the shape and number of roots of the molars which cannot be observed in the mouth directly.
Assessment and special investigations [edit]
A comprehensive history taking should be performed to discover out the pain history of the molar, patient's medical history and history of previous difficult extractions.[one] The tooth should exist assessed clinically i.due east. checked visually by the dentist.[1] Pre-extraction radiographs are not ever necessary just are often taken to confirm the diagnosis and hence advisable treatment programme.[ane] Radiographs also help in visualising the shape and size of roots which are beneficial in planning the extraction.[ane] All this data volition aid the dentist in foreseeing whatsoever difficulties and hence fix appropriately.[1]
Obtaining consent from patient [edit]
In club to obtain permission from patient for extraction of tooth the dentist should explain; other treatment options available, what is involved in the dental extraction procedure, the potential risks of the process and the benefits of the procedure.[1] The procedure of gaining consent should be documented in clinical notes.[1]

Marking Roback, a Navy dentist from the Military Sealift Command (MSC) hospital ship USNSMercy(T-AH-19), speaking to his patient through an interpreter, informs her near the injection he is giving.
Giving local anaesthetic [edit]
Earlier extracting a molar, the dentist would deliver local anaesthetic to ensure the molar and surrounding tissues are numb earlier they commencement the extraction.[1] There are several techniques to achieve numbness of the tooth including
- infiltration - injection containing local anaesthetic is delivered into the gum near the root tip of the tooth to exist extracted. This allows the local anaesthetic to penetrate through the os, eventually reaching the nerve bundle of the tooth to exist extracted.[1]
- nervus block - injection containing local anaesthetic is delivered to an earlier branch of a nervus. For example, the inferior alveolar nerve block can be used to anaesthetise all the lower teeth.[1]
The two most commonly used local anaesthetics in the Uk are lidocaine and articaine.[2] Prior to injection, topical anaesthetic gel or cream, such as lidocaine or benzocaine, can be practical to the gum to numb the site of the injection upwardly to a few millimetres deep.[1] This should reduce the discomfort felt during the injection and thus help to reduce patient anxiety.[1]

Dental extraction forceps.
Removal of tooth [edit]
During extraction, multiple instruments are used to assist and ease the removal of the tooth whilst trying to minimally traumatise the tissues to allow for quicker healing. Extraction forceps are normally used to remove teeth. Dissimilar shaped forceps are available depending on the type of tooth requiring removal, what side of the rima oris (left or correct) it is on and if it is an upper or lower molar. The beaks of the forceps must grip onto the root of the molar securely before pressure is applied forth the long centrality of the tooth towards the root.[1]
Different movements of the forceps can exist employed to remove teeth. By and large, while keeping downwards pressure attempts to move the tooth towards the cheek side (buccal) and and so the opposite direction (palatal or lingual) are made to loosen the molar from its socket.[i] For unmarried, conical-rooted teeth such equally the incisors, rotatory movements are also used.[1] A 'figure of eight' motion can be used to extract lower molars.[1]

Instruments used are summarised below:
| Name | Type of Musical instrument | Use | Surface area of use | Unique features |
|---|---|---|---|---|
| Luxator | Luxator | Tear PDL around molar | Anywhere | Sharp blade |
| Coupland | Elevator | aggrandize socket and lift | Anywhere | Numbered 1-3 from virtually narrow to wide |
| Warrick James | Lift | Aggrandize socket and lift tooth | Anywhere | Correct left and direct |
| Cryers | Elevator | Aggrandize socket and lift molar | Anywhere | Right and left with precipitous tips |
| Upper direct | Forcep | Remove teeth | Upper canine to canine | Directly handle |
| Upper anterior | Forcep | Remove teeth | Upper anteriors and premolars | |
| Upper molar | Forcep | Remove teeth | Upper 1st/2nd/third molars | One pointed cease to appoint buccal furcation |
| Upper bayonet | Forcep | Remove teeth | Upper 3rd molars | Curved handle and tip to attain 3rd molars |
| Upper root | Forcep | Remove teeth | Upper retained/fractured roots | Narrow tips |
| Cowhorn | Forcep | Remove teeth | Lower molars | Thin tips to engage furcation of broken downwardly molars |
| Lower anterior | Forcep | Remove teeth | Lower anteriors and premolars | ninety degree bend handle |
| lower tooth | Forcep | Remove teeth | Lower 1st/2nd/3rd molars | 2 nib tips to appoint furcations |
| Lower root | Forcep | Remove teeth | Lower retained/fractured roots | Narrow tips to engage roots |
In terms of operator positioning when removing a tooth, the patient is placed more supine when extracting and upper and more upright when extracting a lower. This is to allow direct vision for the operator during the procedure. A right handed operator will stand to the forepart of the patient and to their right when removing any upper teeth or lower left teeth. However, they will stand behind the patient and to the right when extracting a lower right tooth.[3]
Dental elevators can be used to aid removal of teeth. Various types are available that have different shapes. Their working ends are designed to engage into the space between the molar and os of the socket.[1] Rotatory movements are then fabricated to dislodge the tooth from the socket.[1] Another similar looking merely sharper instrument that tin be used is a luxator; this instrument tin be used gently and with keen care to cutting the ligament between the molar and its boney socket (periodontal ligament).[ane]
Achieving haemostasis [edit]
Biting down on a piece of sterile gauze over the socket will provide firm pressure level to the wound. Usually this is sufficient to stop any bleeding and will promote blood clot formation at the base of operations of the socket.[4]
The source of any haemorrhage tin can either exist from soft tissues (gingiva and mucosa) or difficult tissue (the bony socket).[iv] Bleeding of soft tissues tin can be controlled past several means including suturing the wound (stitches) and/ or using chemical agents such as tranexamic acid, ferric sulphate and silver nitrate.[4] Bony haemorrhage can be arrested by using haemostatic gauze and bone wax.[4] Other means of achieving haemostasis include electrocautery.[four]
Reasons [edit]


Medical/Dental
- Astringent molar decay or infection (acute or chronic alveolar abscess, such as periapical abscess – collection of infected textile [pus] forming at the tip of the root of a molar).[v] Despite the reduction in worldwide prevalence of dental caries, it is still the most common reason for extraction of (non-third molar) teeth, accounting for up to 2 thirds of extractions.[6]
- Severe mucilage disease, which may touch the supporting tissues and bone structures of teeth.
- Treatment of symptomatic impacted wisdom teeth e.k. that are associated with pericoronitis, unrestorable caries or cysts.[7]
- Safety removal of asymptomatic impacted wisdom teeth. Historically, many asymptomatic impacted third molars were removed, yet, both American and British Health Authorities now provide guidance near the indication for third tooth removal.[7] The American Public Health Association, for example, adopted a policy, Opposition to Prophylactic Removal of 3rd Molars (Wisdom Teeth), because of the large number of injuries resulting from unnecessary extractions.[8]
- Supernumerary teeth that are blocking other teeth from coming in.
- Supplementary or malformed teeth.
- Fractured teeth.
- Cosmetic: to remove teeth of poor advent, unsuitable for restoration.
- Teeth in the fracture line of the jaw bone
- Teeth which cannot exist restored endodontically.
- Prosthetics; teeth detrimental to the fit or advent of dentures.[9]
- Caput and neck radiation therapy, to treat and/or manage tumors, may require extraction of teeth, either before or later radiations treatments.
- Lower cost, compared to other treatments.[x] : 98
- Medically unnecessary extraction as a form of physical torture.[11]
- Information technology was once a common practice to remove the front end teeth of institutionalized psychiatric patients who had a history of biting.[12]
Orthodontic
- In training for orthodontic treatment (braces). Extractions are usually required before the provision of orthodontic treatment, to create infinite for crowded teeth to be moved into. The premolar teeth are the most commonly extracted teeth for this purpose.
Aesthetics
- Cosmetic: to remove teeth of poor appearance, unsuitable for restoration.
Types [edit]

Dental extraction forceps commonly used on teeth in the maxillary arch
Extractions are often categorized equally "unproblematic" or "surgical".
Simple extractions are performed on teeth that are visible in the mouth, usually with the patient nether local anaesthetic, and require merely the use of instruments to drag and/or grasp the visible portion of the molar. Typically the tooth is lifted using an lift, and using dental forceps, specific molar movements are performed (due east.k. rocking the tooth back and forth) expanding the tooth socket. In one case the periodontal ligament is broken and the supporting alveolar bone has been adequately widened the molar can exist removed. Typically, when teeth are removed with forceps, ho-hum, steady pressure is practical with controlled force.

Molar cut upward during surgical extraction - the curvature of the iii roots (top right) prevented simple extraction
Surgical extractions involve the removal of teeth that cannot be easily accessed or removed via uncomplicated extraction, for example considering they have broken under the mucilage or because they take non erupted fully, such equally an impacted wisdom molar.[1] Surgical extractions nigh always require an incision. In a surgical extraction the dentist may drag the soft tissues covering the tooth and bone, and may too remove some of the overlying and/or surrounding jaw bone with a drill or, less commonly, an instrument chosen an osteotome. Often, the tooth may be divide into multiple pieces to facilitate its removal.
Mutual risks after whatsoever extraction include pain, swelling, haemorrhage, bruising, infection, trismus (non being able to open equally wide as normal) and dry out socket. There are boosted risks associated with the surgical extraction of wisdom teeth in particular: permanent or temporary damage to the inferior alveolar nerve +/- lingual nerve, causing permanent or temporary numbness, tingling or altered sensation to the lip, mentum +/- tongue.[13] [14]
Surgical procedure [edit]
- Incisions are fabricated total thickness through mucosa and periosteum to bone. In general, the flap is extended from i molar behind the tooth concerned to one tooth in front, including the interdental papilla.
- An inductive relieving incision is fabricated extending down into the sulcus. This flap blueprint is chosen "two sided". A "three sided" flap includes an additional relieving incision posteriorly.
- The flap is raised using periosteal lift to expose the area of interest.
- The flap is held out of the manner with an instrument such as a rake retractor.
- A small gutter of bone is drilled abroad around the molar to make space into which an awarding signal for instruments can be achieved. It is important that copious amount of saline is used to cool the bone during this process.
- The tooth concerned can be removed using a combination of luxators, elevators and extraction forceps.
- Any sharp os is smoothed off and the wound is irrigated with saline.
- The flap is repositioned and sutured in place.[i]
[edit]
Anticoagulant/Antiplatelet Use [edit]
Anticoagulants are drugs that interfere with the clotting cascade. Antiplatelets are drugs that interfere with platelet aggregation. These drugs are prescribed in certain medical conditions/situations to reduce the gamble of a thromboembolic event. With this comes an increased chance of bleeding. Historically, the anticoagulant warfarin (belonging to the group of drugs called coumarins) and antiplatelets such as aspirin or clopidogrel, were prescribed normally in these circumstances. All the same, whilst these drugs are however used, newer antiplatelet (e.g. ticagrelor) and anticoagulant (east.g. rivaroxaban, apixaban and dabigatran) drugs are being used more than normally. When considering dental handling (including dental extractions) different guidance/precautions need to exist followed depending on the drug prescribed and the individual patient circumstances. The Scottish Dental Clinical Effectiveness Programme (SDCEP) provides splendid guidance on this topic.[fifteen]
Antibiotic Prescribing [edit]
Individual patient circumstances should be evaluated prior to the use of antibiotics to reduce the risks of certain post-extraction complications. At that place is evidence that use of antibiotics before and/or later impacted wisdom tooth extraction reduces the risk of infections past 66%, and lowers incidence of dry socket by i third. For every 19 people who are treated with an antibiotic following impacted wisdom molar removal, one infection is prevented.[xvi] Use of antibiotics does not seem to have a direct effect on manifestation of fever, swelling, or trismus seven days post-extraction. In the 2022 Cochrane review, 23 randomized control double-blinded experiments were reviewed and, later on considering the biased risk associated with these studies, it was concluded that there is moderate overall testify supporting the routine use of antibiotics in practice in order to reduce risk of infection following a third tooth extraction. There are still reasonable concerns remaining regarding the possible adverse effects of indiscriminate antibody use in patients. There are also concerns about development of antibiotic resistance which advises against the use of safe antibiotics in practice.[16] Therefore, given that the risks of antibiotics demand to be counterbalanced against the possible side effects/adverse effects, antibiotics are not routinely prescribed before or after a dental extraction.
Assessing gamble of nerve harm [edit]
The junior alveolar nervus (IAN), a branch of the trigeminal nerve (cranial nerve V), is a nerve that runs through the mandible (lower jaw) and supplies awareness to all the lower teeth, the lip and the chin. The lower teeth, and in particular the lower wisdom teeth, tin can therefore be in close proximity to this nerve. Damage to the inferior alveolar nerve is a risk of lower wisdom molar removal (and other surgical procedures in the mandible).[17] This means at that place is a risk of temporary or permanent numbness or altered sensation to the lip +/- mentum on the side the surgery is taking identify. Therefore, in order to assess this risk and inform the patient, the position of the inferior alveolar nervus in relation to a lower wisdom tooth needs to be assessed radiographically prior to extraction.[17]
The proximity of the root to the canal can be assessed radiographically and in that location are several factors which tin indicate high risk of nerve damage:[18]
- Darkening of the tooth root where it crosses the canal[eighteen]
- Divergence of the canal[xviii]
- Narrowing of the roots[18]
- Loss of the lamina dura of the canal[xviii]
- Juxta apical area: a radiolucency associated with the root of the tooth which is not acquired by periapical infection[eighteen]
The lingual nerve can also be damaged (temporary or permanent) during surgical procedures in the mandible, in particular lower wisdom tooth removal. This would present as temporary or permanent numbness/altered awareness/altered taste to the side of natural language (side respective to side of surgery).[19]
[edit]

Exodontia of first molar, one hour subsequently.
Immediate management [edit]
Immediately following the removal of a molar, bleeding or oozing very commonly occurs. Pressure is practical by the patient biting on a gauze swab, and a thrombus (claret clot) forms in the socket (hemostatic response). Mutual hemostatic measures include local pressure awarding with gauze, and the utilize of oxidized cellulose (gelfoam) and fibrin sealant. Dental practitioners commonly take absorbent gauze, hemostatic packing fabric (oxidized cellulose, collagen sponge), and suture kit bachelor.[20] Sometimes 30 minutes of continuous pressure is required to fully arrest haemorrhage.
Complications [edit]
Talking, which moves the mandible and hence removes the pressure applied on the socket, instead of keeping constant pressure, is a very common reason that bleeding might non stop. This is likened to someone with a bleeding wound on their arm, when being instructed to apply force per unit area, instead holds the wound intermittently every few moments.
Coagulopathies (clotting disorders, east.g. hemophilia) are sometimes discovered for the first time if a person has had no other surgical procedure in their life, merely this is rare. Sometimes the blood clot can be dislodged, triggering more bleeding and formation of a new blood clot, or leading to a dry socket (run across complications). Some oral surgeons routinely scrape the walls of a socket to encourage bleeding in the belief that this will reduce the chance of dry socket, but at that place is no evidence that this practice works.[ citation needed ]
The well-nigh serious post extraction healing complication is that slow or halted healing caused by the adverse effects of use of bisphosphonates which tin cause osteochemonecrosis of the bone.
Healing process [edit]
The chance of further bleeding reduces equally healing progresses, and is unlikely after 24 hours. The blood clot is covered by epithelial cells which proliferate from the gingival mucosa of socket margins, taking most x days to fully cover the defect.[21] In the clot, neutrophils and macrophages are involved every bit an inflammatory response takes place. The proliferative and synthesizing phase next occurs, characterized by proliferation of osteogenic cells from the adjacent bone marrow in the alveolar os. Bone formation starts after about x days from when the tooth was extracted. Afterward 10–12 weeks, the outline of the socket is no longer credible on an X-ray epitome. Bone remodeling equally the alveolus adapts to the edentulous state occurs in the longer term as the alveolar procedure slowly resorbs. In maxillary posterior teeth, the degree of pneumatization of the maxillary sinus may likewise increase as the antral floor remodels.[ citation needed ] [ clarification needed ]
[edit]
Post-extraction bleeding is bleeding that occurs 8–12 hours after tooth extraction.[22]
Factors [edit]
Various factors contribute to post-extraction bleeding.[23] [24] [25]
Local factors
- Laceration of blood vessels
- Osseous bleeding from nutrients culvert/ central vessels
- Inflammation
- Infection
- Traumatic extraction
- Failure of patient to follow post-extraction instructions
Systemic factors
- Platelet problem
- Coagulation disorder/ excessive fibrinolysis
- Inherited/medication-induced problems
Type of bleeding [edit]
1. Main prolonged bleeding
This type of bleeding occurs during/immediately after extraction, because truthful haemostasis has non been accomplished. Information technology is ordinarily controlled by conventional techniques, such every bit applying force per unit area packs or haemostatic agents onto the wound.
ii. Reactionary bleeding
This type of bleeding starts 2 to three hours subsequently tooth extraction, as a issue of cessation of vasoconstriction. Systemic intervention might be required.
3. Secondary bleeding
This type of bleeding normally begins 7 to 10 days mail service extraction, and is near probable due to infection destroying the claret clot or ulcerating local vessels.
Interventions [edit]
There is no clear prove from clinical trials comparing the effects of unlike interventions for the treatment of post-extraction haemorrhage.[26] In view of the lack of reliable show, clinicians must use their clinical experience to determine the most appropriate means of treating this condition, depending on patient-related factors.[26]
Complications [edit]
- Infection: The dentist may opt to prescribe antibiotics pre- and/or post-operatively if he or she determines the patient to be at run a risk of infection.[27]
- Prolonged bleeding: The dentist has a variety of means at his disposal to address bleeding; however, small amounts of claret mixed in the saliva afterwards extraction are normal, even up to 72 hours later extraction. Usually, nevertheless, haemorrhage volition almost completely cease within viii hours of the surgery, with only minuscule amounts of blood mixed with saliva coming from the wound. A gauze compress will significantly reduce bleeding over a period of a few hours.[28]

Example of post-operative swelling following third molar (wisdom teeth) extractions.
- Swelling: Often dictated by the amount of surgery performed, to extract a tooth (e.g., surgical insult to the tissues, both difficult and soft, surrounding a tooth). Generally, when a surgical flap must be elevated (i.e., the periosteum roofing the bone is thus injured), minor to moderate swelling volition occur. A poorly cut soft tissue flap, for instance, where the periosteum is torn off rather than cleanly elevated off the underlying bone, will often increase such swelling. Similarly, when bone must be removed using a drill, more swelling is likely to occur.
- Bruising: Bruising may occur as a complication after tooth extraction.[29] Bruising is more than mutual in older people or people on aspirin or steroid therapy. It may accept weeks for bruising to disappear completely.
- Sinus exposure and oral-antral communication: This tin occur when extracting upper molars (and in some patients, upper pre-molars). The maxillary sinus sits directly higher up the roots of maxillary molars and pre-molars. There is a bony floor of the sinus, dividing the tooth socket from the sinus itself. This bone can range from thick to thin, from tooth to tooth, from patient to patient. In some cases it is absent and the root is, in fact, in the sinus. At other times, this bone may be removed with the tooth, or may be perforated during surgical extraction. The doctor typically mentions this risk to patients, based on evaluation of radiographs showing the relationship of the tooth to the sinus. The sinus cavity is lined with a membrane called the Sniderian membrane, which may or may not be perforated. If this membrane is exposed later an extraction, just remains intact, a "sinus exposed" has occurred. If the membrane is perforated, all the same, it is a "sinus communication". These two conditions are treated differently. In the event of a sinus advice, the dentist may decide to permit information technology heal on its ain, or, may need to surgically obtain primary closure—depending on the size of the exposure and the likelihood of the patient to heal. In both cases, a resorbable fabric called "gelfoam" is typically placed in the extraction site to promote clotting and serve every bit a framework for granulation tissue to accumulate. Patients are typically provided with prescriptions for antibiotics that cover sinus bacterial flora, decongestants, and careful instructions to follow during the healing period.[30]
- Nervus injury: This is primarily an upshot with extraction of tertiary molars, but can occur with the extraction of any tooth should the nerve exist close to the surgical site. Two nerves are typically of business, and are found in indistinguishable (i left and one correct): 1. the junior alveolar nerve, which enters the mandible at the mandibular foramen and exits the mandible at the sides of the mentum from the mental foramen.[31] This nervus supplies awareness to the lower teeth on the right or left one-half of the dental arch, also as sense of touch on to the right or left half of the chin and lower lip. 2. The lingual nervus (one right and one left), which branches off the mandibular branches of the trigeminal nervus and courses simply inside the jaw bone, entering the tongue and supplying sense of bear upon and taste to the right and left half of the anterior 2/3 of the tongue likewise as the lingual gingiva (i.e., the gums on the inside surface of the dental arch). Such injuries tin occur while lifting teeth (typically the inferior alveolar), simply are nearly commonly caused past inadvertent damage with a surgical drill. Such injuries are rare and are ordinarily temporary, only depending on the blazon of injury (i.e., Seddon classification: neuropraxia, axonotmesis, & neurotmesis), tin be prolonged or even permanent.[32]
- Displacement of tooth or part of the tooth into the maxillary sinus (upper teeth only). In such cases, the molar or molar fragment must near always be retrieved. In some cases, the sinus cavity tin be irrigated with saline (antral lavage) and the tooth fragment may exist brought back to the site of the opening through which it entered the sinus, and may exist retrievable. At other times, a window must be fabricated into the sinus in the Canine fossa—a procedure referred to equally a "Caldwell-Luc".[33]

Alveolar osteitis of a socket later molar extraction. Note lack of claret clot in socket and exposed alveolar bone.
- Dry out-socket (Alveolar osteitis) is a painful phenomenon that about unremarkably occurs a few days after the removal of mandibular (lower) wisdom teeth. It typically occurs when the blood clot within the healing tooth extraction site is disrupted. More probable,[34] alveolar osteitis is a phenomenon of painful inflammation inside the empty tooth socket because of the relatively poor blood supply to this expanse of the mandible (which explains why dry-socket is usually not experienced in other parts of the jaw). Inflamed alveolar bone, unprotected and exposed to the oral surround afterward molar extraction, can go packed with food and debris. Dry-socket typically causes a sharp and sudden increase in pain commencing 2–five days post-obit the extraction of a mandibular tooth, most commonly the third molar.[35] This is often extremely unpleasant for the patient; the only symptom of dry-socket is hurting, which often radiates up and downwardly the head and cervix. A dry-socket is not an infection, and is not directly associated with swelling because information technology occurs entirely within bone – it is a phenomenon of inflammation, within the bony lining, of an empty tooth socket. Because dry-socket is non an infection, the use of antibiotics has no consequence on its rate of occurrence. There is some show that rinsing with chlorhexidine before or after extraction or placing chlorhexidine gel in the sockets of extracted teeth provides a do good in preventing dry out-socket, but potential adverse effects of chlorhexidine have to be considered.[36] The risk cistron for alveolar osteitis can dramatically increase with smoking after an extraction.
- Bone fragments: Specially when extraction of molars is involved, it is not uncommon for the bones which formerly supported the tooth to shift and in some cases to erupt through the gums, presenting protruding sharp edges which can irritate the tongue and crusade discomfort. This is distinguished from a like miracle, where, broken fragments of bone or tooth left over from the extraction can likewise protrude through the gums. In the latter example, the fragments will commonly work their way out on their ain. In the one-time example, the protrusions can either be snipped off by the dentist, or somewhen the exposed bone volition erode away on its own.
- Maxilla tuberosity fracture: Can occur especially during tooth extractions. In that location can be a variety of factors causing this including single standing molar, extracting in the wrong order, inadequate alveolar support, pathological gemination or extension of maxillary sinus weakening the area.[37]
- Trismus: Trismus, also known as lockjaw, affects functions of the oral cavity past restricting opening of the mouth. A double bullheaded, clinical report was done to test the effect of two dissimilar medications on postal service-extraction trismus. The patients who received a corticosteroid by IV had a statistically significant lower level of trismus when compared to patients receiving an NSAID past 4 or no medication.[38]
- Loss of a tooth: If an extracted tooth slips out of the forceps, it may be swallowed or inhaled. The patient may be aware of swallowing it, or, they may coughing, which suggests inhalation of the tooth. The patient must be referred for a breast 10-ray in hospital if a tooth cannot be found. If it has been swallowed, no action is necessary as it commonly passes through the alimentary canal without doing whatever harm. Merely if information technology has been inhaled, an urgent functioning is necessary to recover information technology from the airway or lung before information technology causes serious complications such as pneumonia or a lung abscess.[9]
- Luxation of the next tooth: The awarding of forcefulness during the extraction procedure must strictly be limited to the tooth that requires the extraction. Most cases of surgical extraction procedures require that the forces are diverted from the molar itself to areas such as bone surrounding the tooth to ensure adequate bone removal before proceeding any further in the extraction procedure. Either way, the forces applied by various instruments during both elementary and complicated surgical procedure may loosen the teeth present both in front end of or behind the tooth depending upon the affect direction and location of the force existence applied and that happening only if the forces divert from the actual molar that needs extraction. Such deleterious forces may weaken the anchorage of adjacent teeth from inside their bony socket, and hence issue in weakening of the adjacent teeth.
- Extraction of the wrong tooth: Misdiagnosis, contradistinct tooth morphology, faulty clinical examination, poor patient history, undetected/unmentioned previous extractions that may predispose the operator to consider another molar to be a replicate of the one previously extracted are a few causes of extraction of a wrong tooth.
- Osteonecrosis: Osteonecrosis of the jaw is the slow destruction of bone in an extraction site. A case control study of 191 cases and 573 controls were used to understand the relationship between osteonecrosis of the jaw and prior usage of bisphosphonate drugs, which are commonly prescribed to treat osteoporosis. All of the participants were over 40 years of age, by and large female person, and had been taking bisphosphonates for six months or longer. The presence of osteonecrosis of the jaw was reported by dentists' previous diagnosis of the participating case and command patient's medical records. Reports showed that women using bisphosphonates for more two years are x times more likely to experience osteonecrosis of the jaw, while women who have taken bisphosphonates for less than two years are four times more likely to suffer from osteonecrosis of the jaw when compared to women who were not taking bisphosphonates. Therefore, information technology is extremely important to report all medications used to the dentist before an extraction, and then that osteonecrosis tin can be avoided.[39]
[edit]
Pain direction [edit]
Many drug therapies are available for pain management later tertiary molar extractions including NSAIDS (not-steroidal anti-inflammatory), APAP (acetaminophen), and opioid formulations. Although each has its own hurting-relieving efficacy, they besides pose adverse effects. According to ii doctors, Ibuprofen-APAP combinations have the greatest efficacy in pain relief and reducing inflammation along with the fewest adverse furnishings. Taking either of these agents alone or in combination may be contraindicated in those who have certain medical conditions. For example, taking ibuprofen or any NSAID in conjunction with warfarin (a claret thinner) may not be appropriate. Also, prolonged apply of ibuprofen or APAP has gastrointestinal and cardiovascular risks.[40] There is high quality evidence that ibuprofen is superior to paracetamol in managing postoperative pain.[41]
Socket preservation [edit]
Socket preservation or alveolar ridge preservation (ARP)[42] is a process to reduce bone loss afterwards tooth extraction to preserve the dental air sac (tooth socket) in the alveolar bone. At the fourth dimension of extraction a platelet rich fibrin (PRF)[43] membrane containing bone growth enhancing elements is placed in the wound or a graft material or scaffold is placed in the socket of the extracted tooth.[44] [45] The socket is then direct closed with stitches or covered with a non-resorbable or resorbable membrane and sutured.
[edit]
Atraumatic extraction is a novel technique for extracting teeth with minimal trauma to the bone and surrounding tissues. It is especially useful in patients who are highly susceptible to complications such as bleeding, necrosis, or jaw fracture. It can also preserve bone for subsequent implant placement.[46] Techniques involve minimal use of forceps, which damage socket walls, relying instead on luxators, elevators and syndesmotomy.[ citation needed ] [47]
Replacement options for missing teeth [edit]
Following dental extraction, a gap is left. The options to fill this gap are commonly recorded as Demark, and the pick is made by dentist and patient based on several factors.
| Handling option | Advantages | Disadvantages |
|---|---|---|
| Bridge | Fixed to adjacent teeth | Drilling usually required on i or both sides of the gap if conventional bridge (average lifespan about 10 years). Conservative span (average lifespan about 5 years) grooming may crusade minimal damage to next teeth. Expensive and complex treatment, not suited to all situations, east.g., large gaps in the dorsum of the oral fissure Alveolar os volition still resorb, and somewhen a gap may show under bridge. |
| Implant | Fixed to jawbone. Maintains alveolar os, which would otherwise undergo resorption. Usually a long-term lifespan. | Expensive and complex, requiring specialist. May involve other procedures such as bone grafting. Relatively contra-indicated in tobacco smokers. |
| Denture | Often a simple, quick, and relatively cheap treatment compared to bridge and implant. Not ordinarily whatever drilling of other teeth required. Information technology is far easier to replace several teeth with a denture than place multiple bridges or implants. | Denture is not stock-still in rima oris. Over time worsens periodontal disease unless at that place is good level of oral hygiene, and may damage soft tissues. Potential for slightly accelerated resorption of alveolar bone compared to no denture. Potential for poor tolerance in persons with over-sensitive gag reflex, xerostomia, etc. |
| Zippo (i.e., not replacing the missing tooth) | Oftentimes the choice due to cost of other treatment or lack of motivation for other treatments. Office of a shortened dental arch plan, which revolves around the fact that not all teeth are required to swallow comfortably, and simply the incisors and premolars demand exist preserved for normal function. This is ordinarily the choice taken if the reason of dental extraction is due to impacted wisdom teeth or orthodontics because of limited space. | The alveolar bone will slowly resorb over fourth dimension once the tooth is lost. Potential esthetic concern. Potential for globe-trotting and rotation of next teeth into the gap over time. |
History [edit]
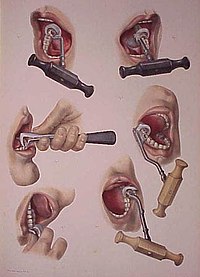
illustration demonstrating the utilize of the dental fundamental for extracting teeth.
Historically, dental extractions accept been used to treat a variety of illnesses. Before the discovery of antibiotics, chronic tooth infections were often linked to a multifariousness of health issues, and therefore removal of a diseased tooth was a common treatment for various medical weather condition. Instruments used for dental extractions engagement back several centuries. In the 14th century, Guy de Chauliac invented the dental pelican,[48] which was used through the late 18th century. The pelican was replaced past the dental key[49] which, in plow, was replaced by modern forceps in the 19th century.[fifty] As dental extractions can vary tremendously in difficulty, depending on the patient and the molar, a wide variety of instruments exist to address specific situations. Rarely, tooth extraction was used every bit a method of torture, e.g., to obtain forced confessions.[51]
See also [edit]
- Tooth regeneration
- Dental evulsion
References [edit]
- ^ a b c d eastward f g h i j k l one thousand n o p q r s t u Pedlar J, Frame JW (2001). Oral and maxillofacial surgery : an objective-based textbook. Edinburgh: Churchill Livingstone. ISBN978-0-443-06017-5. OCLC 45708690.
- ^ Bartlett Yard, Mansoor J (Feb 2016). "Articaine buccal infiltration vs lidocaine inferior dental block - a review of the literature". British Dental Journal. 220 (3): 117–xx. doi:10.1038/sj.bdj.2016.93. PMID 26868800. S2CID 3343775.
- ^ Wray, David (2003). Textbook of General and Oral Surgery. Edinburgh: Churchill Livingston. pp. 208–211. ISBN0443070830.
- ^ a b c d e McCormick NJ, Moore UJ, Meechan JG (May 2014). "Haemostasis. Part 1: The direction of post-extraction haemorrhage". Dental Update. 41 (4): 290–2, 294–six. doi:ten.12968/denu.2014.41.4.290. PMID 24930250.
- ^ Karagianis A (2016-03-22). Caput and Neck Imaging Variants. ISBN9780071808682.
- ^ Zadik Y, Sandler V, Bechor R, Salehrabi R (November 2008). "Analysis of factors related to extraction of endodontically treated teeth". Oral Surgery, Oral Medicine, Oral Pathology, Oral Radiology, and Endodontics. 106 (5): e31-5. doi:x.1016/j.tripleo.2008.06.017. PMID 18718782.
- ^ a b Guidance on the Extraction of Wisdom Teeth. National Institute of Clinical Excellence. 27 March 2000. ISBN9781473131484.
- ^ "Opposition to Safe Removal of Tertiary Molars (Wisdom Teeth)". Policy Statement Database. American Public Health Clan. 2016-05-12. Retrieved 2016-05-12 .
- ^ a b Hollins C (2008). Levison'southward Textbook for Dental Nurses. ISBN978-1-4051-7557-9.
- ^ Hupp JR, Ellis E, Tucker MR (2008). Gimmicky oral and maxillofacial surgery (5th ed.). St. Louis, Mo.: Mosby Elsevier. ISBN9780323049030.
- ^ Speers RD, Brands WG, Nuzzolese Eastward, Smith D, Swiss Lead, van Woensel M, Welie JV (December 2008). "Preventing dentists' interest in torture: the developmental history of a new international announcement". Journal of the American Dental Clan. 139 (12): 1667–73. doi:10.14219/jada.archive.2008.0109. PMID 19047673. S2CID 22188815.
- ^ C. Thomas Gualtieri (2002). Brain injury and mental retardation: psychopharmacology and neuropsychiatry. ISBN9780781734738.
- ^ Sarikov R, Juodzbalys M (2014-12-29). "Junior alveolar nerve injury subsequently mandibular third molar extraction: a literature review". Journal of Oral & Maxillofacial Research. v (4): e1. doi:10.5037/jomr.2014.5401. PMC4306319. PMID 25635208.
- ^ Malden NJ, Maidment YG (Baronial 2002). "Lingual nerve injury subsequent to wisdom teeth removal--a five-yr retrospective audit from a high street dental exercise". British Dental Journal. 193 (four): 203–five. doi:10.1038/sj.bdj.4801523. PMID 12222906.
- ^ "Management of Dental Patients Taking Anticoagulants or Antiplatelet Drugs" (PDF). Scottish Dental Clinical Effectiveness Programme.
- ^ a b Lodi, Giovanni; Azzi, Lorenzo; Varoni, Elena Maria; Pentenero, Monica; Del Fabbro, Massimo; Carrassi, Antonio; Sardella, Andrea; Manfredi, Maddalena (2021-02-24). "Antibiotics to prevent complications following tooth extractions". The Cochrane Database of Systematic Reviews. ii: CD003811. doi:10.1002/14651858.CD003811.pub3. ISSN 1469-493X. PMC8094158. PMID 33624847.
- ^ a b Juodzbalys K, Daugela P (July 2013). "Mandibular third molar impaction: review of literature and a proposal of a classification". Periodical of Oral & Maxillofacial Research. 4 (two): e1. doi:10.5037/jomr.2013.4201. PMC3886113. PMID 24422029.
- ^ a b c d due east f Renton, Tara (2013-06-02). "Update on coronectomy. a safer mode to remove high adventure mandibular 3rd molars". Dental Update. 40 (5): 362–368. doi:x.12968/denu.2013.40.5.362. ISSN 0305-5000. PMID 23909229.
- ^ Renton, T. (October 2013). "Oral surgery: part iv. Minimising and managing nerve injuries and other complications". British Dental Journal. 215 (eight): 393–399. doi:10.1038/sj.bdj.2013.993. ISSN 0007-0610. PMID 24157759.
- ^ "Management of Dental Patients taking Anticoagulant or Anti Platelet Drug" (PDF).
- ^ Antonio N, ed. (2007). Oral histology: development, structure, and part (7th ed.). St. Louis, Mo.: Mosby. ISBN9780323045575.
- ^ Kumbargere Nagraj South, Prashanti Eastward, Aggarwal H, Lingappa A, Muthu MS, Kiran Kumar Krishanappa S, Hassan H (March 2018). "Interventions for treating post-extraction bleeding". The Cochrane Database of Systematic Reviews. iii: CD011930. doi:x.1002/14651858.CD011930.pub3. PMC6494262. PMID 29502332.
- ^ Ramos E, Santamaría J, Santamaría Thousand, Barbier Fifty, Arteagoitia I (October 2016). "Do systemic antibiotics forbid dry out socket and infection after third molar extraction? A systematic review and meta-analysis". Oral Surgery, Oral Medicine, Oral Pathology and Oral Radiology. 122 (4): 403–25. doi:10.1016/j.oooo.2016.04.016. PMID 27499028.
- ^ McCormick NJ, Moore UJ, Meechan JG (May 2014). "Haemostasis. Part one: The management of mail service-extraction bleeding". Dental Update. 41 (4): 290–2, 294–6. doi:10.12968/denu.2014.41.4.290. PMID 24930250. S2CID 4237610.
- ^ Mitchell 50, McCaul Fifty, Mitchell DA (2009). Oxford handbook of clinical dentistry (fifth ed.). Oxford: Oxford University Press. ISBN978-0199553303. OCLC 316027998.
- ^ a b Kumbargere Nagraj S, Prashanti E, Aggarwal H, Lingappa A, Muthu MS, Kiran Kumar Krishanappa Southward, Hassan H (March 2018). "Interventions for treating post-extraction bleeding". The Cochrane Database of Systematic Reviews. John Wiley & Sons, Ltd. iii: CD011930. doi:10.1002/14651858.cd011930.pub3. PMC6494262. PMID 29502332.
- ^ Yue Yi EK, Siew Ying AL, Mohan Chiliad, Menon RK. Prevalence of Postoperative Infection later Tooth Extraction: A Retrospective Report. Int J Dent. 2021;2021:6664311. Published 2022 Jun 8. doi:10.1155/2021/6664311
- ^ Kumbargere Nagraj South, Prashanti Due east, Aggarwal H, et al. Interventions for treating post-extraction bleeding. Cochrane Database Syst Rev. 2018;3(3):CD011930. Published 2022 Mar four. doi:ten.1002/14651858.CD011930.pub3
- ^ Susarla, Srinivas (March 2005). "Third tooth surgery and associated complications". Oral and Maxillofacial Surgery Clinics of North America. 15: 177–186 – via Elsevier Science Direct.
- ^ Pierse DMD, Joseph (Jan 2012). "Diagnosis and Direction of Common Postextraction Complications". Dental Clinics of North America. 56: 75–93.
- ^ Sarikov R, Juodzbalys G. Junior alveolar nerve injury afterward mandibular third tooth extraction: a literature review. J Oral Maxillofac Res. 2014;5(four):e1. Published 2022 December 29. doi:ten.5037/jomr.2014.5401
- ^ Coulthard P, Kushnerev E, Yates JM, Walsh T, Patel Due north, Bailey E, Renton TF. Interventions for iatrogenic inferior alveolar and lingual nerve injury. Cochrane Database of Systematic Reviews 2014, Event 4. Art. No.: CD005293. DOI: 10.1002/14651858.CD005293.pub2. Accessed 25 February 2022.
- ^ Seigneur, Mathilde (26 August 2020). "Teeth roots deportation in the maxillary sinus: characteristics and direction". Journal of Oral Medicine and Oral Surgery. 26: 9.
- ^ Kolokythas A, Olech East, Miloro 1000 (2010). "Alveolar osteitis: a comprehensive review of concepts and controversies". International Periodical of Dentistry. 2010: 249073. doi:ten.1155/2010/249073. PMC2905714. PMID 20652078.
- ^ Daly B, Sharif MO, Newton T, Jones Chiliad, Worthington HV (December 2012). "Local interventions for the direction of alveolar osteitis (dry out socket)". The Cochrane Database of Systematic Reviews. 12: CD006968. doi:10.1002/14651858.CD006968.pub2. PMID 23235637.
- ^ Dodson T (March 2013). "Prevention and handling of dry out socket". Evidence-Based Dentistry. 14 (1): 13–4. doi:10.1038/sj.ebd.6400913. PMID 23579300.
- ^ Polat, Hidayet (October 2007). "Maxillary Tuberosity Fracture Associated with First Molar Extraction: A Example Report". European Periodical of Dentistry: 256–259.
- ^ Ilhan O, Agacayak KS, Gulsun B, Koparal M, Gunes N (January 2014). "A comparison of the effects of methylprednisolone and tenoxicam on pain, edema, and trismus subsequently impacted lower 3rd molar extraction". Medical Science Monitor. 20: 147–52. doi:x.12659/MSM.890239. PMC3915002. PMID 24473372.
- ^ Barasch A, Cunha-Cruz J, Curro FA, Hujoel P, Sung AH, Vena D, et al. (Apr 2011). "Risk factors for osteonecrosis of the jaws: a example-control study from the CONDOR dental PBRN". Journal of Dental Inquiry. 90 (4): 439–44. doi:10.1177/0022034510397196. PMC3144129. PMID 21317246.
- ^ Moore PA, Hersh EV (August 2013). "Combining ibuprofen and acetaminophen for acute pain management afterwards 3rd-molar extractions: translating clinical enquiry to dental practice". Journal of the American Dental Association. 144 (8): 898–908. doi:10.14219/jada.annal.2013.0207. PMID 23904576.
- ^ Bailey Due east, Worthington HV, van Wijk A, Yates JM, Coulthard P, Afzal Z (December 2013). "Ibuprofen and/or paracetamol (acetaminophen) for pain relief later surgical removal of lower wisdom teeth". The Cochrane Database of Systematic Reviews (12): CD004624. doi:10.1002/14651858.CD004624.pub2. PMID 24338830.
- ^ Peck MT, Marnewick J, Stephen Fifty (2011). "Alveolar ridge preservation using leukocyte and platelet-rich fibrin: a written report of a example". Case Reports in Dentistry. 2011: 345048. doi:10.1155/2011/345048. PMC3335652. PMID 22567435.
- ^ Khiste SV, Naik Tari R (2013). "Platelet-Rich Fibrin every bit a Biofuel for Tissue Regeneration". ISRN Biomaterials. 2013: one–vi. doi:10.5402/2013/627367. ISSN 2314-4025.
- ^ Irinakis T (December 2006). "Rationale for socket preservation subsequently extraction of a unmarried-rooted molar when planning for future implant placement" (PDF). Periodical (Canadian Dental Association). 72 (10): 917–22. PMID 17187706.
- ^ Fickl Southward, Zuhr O, Wachtel H, Stappert CF, Stein JM, Hürzeler MB (October 2008). "Dimensional changes of the alveolar ridge contour after different socket preservation techniques". Journal of Clinical Periodontology. 35 (10): 906–xiii. doi:10.1111/j.1600-051X.2008.01305.ten. PMID 18713258. S2CID 4954931.
- ^ Tavarez RR, Dos Reis WL, Rocha AT, Firoozmand LM, Bandéca MC, Tonetto MR, Malheiros AS (Dec 2013). "Atraumatic extraction and immediate implant installation: The importance of maintaining the profile gingival tissues". Journal of International Oral Health. 5 (six): 113–8. PMC3895728. PMID 24453455.
- ^ Syndesmotomy; medical-lexicon.the freedictionary.com; accessed 2020-08-27
- ^ "Dental pelican for tooth pulling, Europe, 1701–1800". sciencemuseum.org.britain. Brought to Life. Retrieved 18 February 2014.
- ^ Ribitzky G. "Toothkey". Retrieved 23 June 2018.
- ^ Ribitzky M. "Forceps". Retrieved 23 June 2018.
- ^ Claude RP, Weston BH (2006). Human rights in the world community : issues and action (3rd ed.). Philadelphia: University of Pennsylvania Press. p. 91. ISBN9780812219487.
Further reading [edit]
- "Tooth Extraction". American Dental Association. 2013-09-06. Archived from the original on 2021-12-21.
External links [edit]
Source: https://en.wikipedia.org/wiki/Dental_extraction
0 Response to "Use Extraction Operator to Read in File"
Enviar um comentário